What is TRANSPOSITION of the GREAT ARTERIES (TGA)?
The great arteries represent the aorta and pulmonary artery. With normal status quo, the pulmonary artery connects to the lower right chamber, or right ventricle of the heart. Blood is pumped from the lower right chamber via the pulmonary artery to the lungs. The left ventricle, or left lower chamber pumps blood via the aorta (main artery leading from the left ventricle) to the rest of the body.
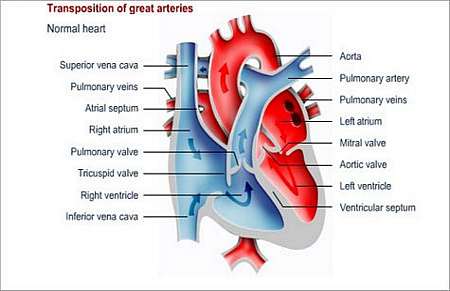
In a child with this condition, the great arteries are reversed from their normal connections/position. This means that the aorta (main artery that takes blood to the rest of the body), which normally comes off the left ventricle, comes off the right ventricle and pumps blue blood, returning from the body, back to the body bypassing the lungs completely. On the other hand, the pulmonary artery, which normally arises from the right ventricle and is responsible for pumping blue blood to the lungs, arises from the left ventricle and sends red blood, returning from the lungs, right back to the lungs.
Therefore, unoxygenated blood (dark blue blood without oxygen that comes from the right ventricle) is being pumped through the body and red (oxygenated) blood is pumped to the lungs and not to the rest of the body.
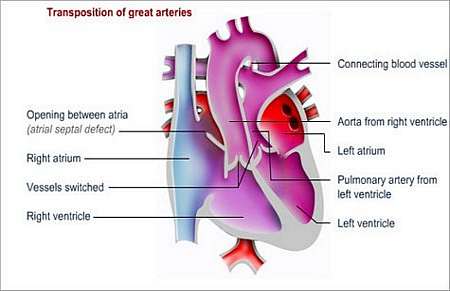
Oxygen-rich blood can only reach the body via another defect that connects the two routes e.g.
- An atrial septal defect (ASD) (hole in the septum that separates the left and right upper heart chambers), which allows for the exchange of blood between the two atria, or a
- Ventricular septal defect, which allows for exchange of blood between the two ventricles (lower heart chambers), or a
- Patent ductus arteriosus (a temporary blood vessel that connects the pulmonary artery and the aorta); the ductus arteriosus is open before the baby is born and usually closes in the first few days of the babys life
What symptoms may the patient experience?
Symptoms appear very early in life (usually in the first few days). The baby appears cyanotic (blue discoloration of skin) with symptoms of difficult breathing and poor feeding.
The babys survival depends on how much red (oxygen-rich) and blue (without oxygen) blood mix together within the heart to circulate through the body. One of the three above-mentioned defects, or combinations thereof, may allow sufficient mixing, so that enough oxygen may reach the rest of the body. If the opening(s) between the two sides of the heart are large enough, symptoms will only appear at a later stage.
How is the diagnosis made and what special investigations are required?
What is the treatment?
A newborn baby may be treated with medicine that will keep the ductus arteriosus open. This is necessary in order to allow oxygen-rich blood to reach the systemic circulation (the body), because the ductus usually starts to close soon after birth.
- Balloon septostomy
When there is no other defect, such as and atrial septal defect or ventricular septal defect, doctors will create an artificial atrial septal defect by means of a balloon septostomy. A balloon tipped catheter (a fine hollow tube with a balloon at the tip) is used to create a hole in the wall separating the left and right upper heart chambers. This procedure will suffice until an arterial switch operation can be performed. The medicines and the balloon septostomy are only short-term solutions, which fulfil a critical role by allowing the body to get oxygen-rich blood until such time as surgery can be performed to correct the transposition.
- Arterial switch operation
During this procedure, the aorta and the pulmonary artery are disconnected and switched (reversed) to the correct position. The pulmonary artery is connected to the right ventricle and the aorta is connected to the left ventricle. The coronary arteries that supply blood to the heart also have to be switched. Any holes within the heart will be repaired at the same time as this operation.
Most children with TGA undergo this operation, which is mostly done within the first four weeks of the childs life. A heart-lung machine is used during this operation.
The patient will require regular outpatient check-ups after the operation.
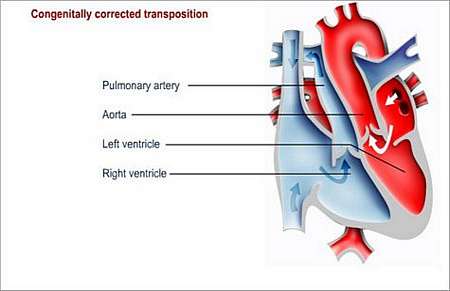
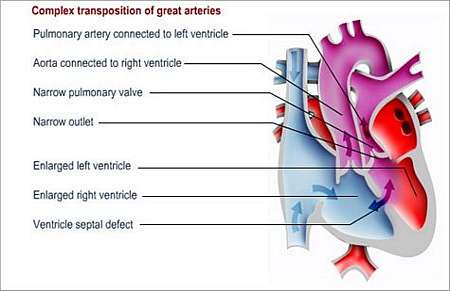
Complex variations (especially when involving the left ventricle outflow tract), for which other surgical options will have to be considered, exist.
Preventing endocarditis
It is important to take measures to prevent endocarditis for the rest of the childs life. Endocarditis is an infection of the lining of the heart or heart valves.
The child should wear a Medic Alert card/bracelet stating the need for antibiotics before certain forms of surgery or dentistry.
© 2003 Prometheus™ Healthcare (Pty) Ltd
|